Management of Sexually Transmitted Infections by Community Pharmacists in Lagos, Nigeria: a Cross-sectional Study
Keywords:
Sexually Transmitted, Infections, symptoms, Community Pharmacists, Lagos, NigeriaAbstract
Background: Sexually Transmitted Infections (STIs) are of public health importance in Nigeria. Timely interventions could alleviate STI-associated symptoms, and delay transmission. This study investigated how Community Pharmacists responded to complaints of STI-associated symptoms and explored factors that hinder these efffforts.
Methods: A cross-sectional, descriptive study was carried out among 48 Community Pharmacists in Surulere Local Government Area of Lagos. Data were collected using a pretested self-administered, semi-structured questionnaire that comprised demographic characteristics of the pharmacists and the patients, STI symptoms, and services provided by the community pharmacists. Descriptive and inferential statistics were used to summarize the data using SPSS version 20.0. AP-value of <0.05 was considered signifificant.
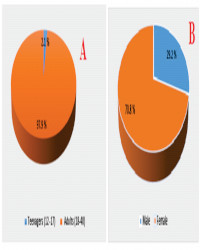
Results: More than half of the Community Pharmacists (58.3%) were females, with 56.3 % having < 5years of practice experience. An average of 10 patients presented to the pharmacies daily with STI associated symptoms. Most patients (97.9%) were aged 18 to 49 years, and are mainly females (70.8%). The most common STI-associated complaints in females were vaginal discharge (93.8%) and urethral discharge (70%) in men. On any STI-related visit, the pharmacist elicited information on the history of present symptoms (92%), medications taken before the pharmacies' visit (88%), onset and duration of symptoms (85%). They suggested medications (94%), counseled patients on medication use (89%), offffered preventive care (Condom use (83.3%); abstinence (31.3%), and referred patients to hospital (79%). Un-resolving symptoms (86.8%) were the main reason for referrals. The Pharmacists failed to confifirm patients' identities and did not follow up with the patients in 45.8% of the visits. They suggested metronidazole (89.6%) most, followed by Azithromycin (85% and Ciproflfloxacin (79%). Patients' reluctance to open up was the main obstacle to the provision of STI management services in the community.
Conclusion: Community pharmacists provided a wide range of STI management services of which treatment, medication counseling, and preventive care are the most common. There is a need for pharmacists to improve on referrals and follow-ups to ensure continuity in care.
References
Marsden EJ, Somwe SW, Chabala C, Soriano JB, Vallès CP, Anchochea J (2016). Knowledge and perceptions of asthma in Zambia: a cross- sectional survey. BMC Pulmonary Medicine. 16(1): 1–8. https://doi.org/10.1186/s12890-016-0195-3
Reddel HK, Bateman ED, Becker A, Boulet L, Cruz AA, Drazen JM, Haahtela T, Hurd SS, Inoue H, de Jongste JC, Lemanske Jr RF, Levy ML,
O'Byrne PM, Paggiaro P, Pedersen SE, Pizzichini E, Soto-Quiroz M, Szefler SJ, Wong GWK, FitzGerald JM (2015). A summary of the new
GINA strategy: a roadmap to asthma control. European Respiratory Journal. 46(3): 622-639. https://doi.org/10.1183/13993003.00853-2015
Global Asthma Report (2018). The Global asthma Report 2018, 1-88. [cited March 7, 2022] Available from:
https://www.globalasthmareport.org
Global Initiative for Asthma (2021). Global strategy for asthma management and prevention, 1-217. [cited March 7, 2022] Available from:
Ndlovu V, Chimbari MJ, Sibanda E (2020). Assessing the nature of asthma in African epidemiological studies: a scoping review
protocol. Systematic Reviews. 9: 230. https://doi.org/10.1186/s13643-020-01491-7
Irfan O, Irfan B, Khan ZA, Tahir M, Sarwar Zubairi AB, Khan, JA (2017). Knowledge about asthma: A cross-sectional survey in 4 major hospitals of Karachi, Pakistan. Journal of Pakistan Medical Association. 67(11): 1787-1790.
Global Initiative for Asthma (2021). World Asthma Day – May 5, 2021. [cited March 7, 2022] Available from: https://ginasthma.org/worldasthma-day-may-5-2021/
Jacome SN, Lopez-Padilla C, Madera D, Polo J, Kim EJ, Dhar S, Wang JJ, Hajizadeh N (2021). Using community priorities and misconceptions
about asthma as a vessel for community-led education among Hispanics. Journal of Asthma. 58(3): 405 - 412. https://doi.org/10.1080/02770903.2019.1692027
Amorha KC, Okpe CL, Dim OF (2018). Knowledge, attitudes and perceived practice towards asthma among pharmacy students in Southern Nigeria. International Journal of Pharmacy and Pharmaceutical Sciences. 10(11): 28-34.
Bontsevich R, Vlasova K, Ketova G, Barysheva V, Luchinina E, Malkina M, Goncharova N, Feoktistova Y (2014). Assessment of senior medical students in the field of bronchial asthma. European Respiratory Journal. 44(Suppl 58): P2795.
Tam-Williams JB, Jones BL (2018). Closing the gap: understanding African American asthma knowledge and beliefs. Annals of Allergy, Asthma & Immunology. 121(4): 458 - 463. https://doi.org/10.1016/j.anai.2018.07.015
Boulet LP, Reddel HK, Bateman E, Pedersen S, FitzGerald JM, O'Byrne, PM (2019). The Global Initiative for Asthma (GINA): 25 years later.
European Respiratory Journal. 54(2): 1900598.https://doi.org/10.1183/13993003.00598-2019
Bridgeman MB, Wilken LA(2020). Essential role of pharmacists in asthma care and management. Journal of Pharmacy Practice. 34(1): 149-162. https://doi.org/10.1177/0897190020927274
Kritikos V, Saini B, Bosnic-Anticevich SZ, Krass I, Shah S, Taylor S, Armour C (2005). Innovative asthma health promotion by rural community
pharmacists: a feasible study. Health Promotion Journal of Australia. 16(1): 69 - 73. https://doi.org/10.1071/HE05069
Amorha KC, Asogwa EQ, Ibenekwu CS, Ogbonna ET, Amorha AO (2021). Knowledge and perception about asthma among students in a Nigerian single-sex secondary school. The Clinical Respiratory Journal. 15(10): 1121-1129. https://doi.org/10.1111/crj.13418
Lim RH, Kobzik L, Dahl M (2010). Risk for asthma in offspring of asthmatic mothers versus fathers: a meta-analysis. PLoS ONE 2010; 5(4):
e10134. https://doi.org/10.1371/journal.pone.0010134
Towns SJ, Van Asperen PP(2009). Diagnosis and management of asthma in adults. The Clinical Respiratory Journal 2009; 3(2): 69-76.
https://doi.org/10.1111/j.1752-699X.2009.00130.x
Rabe KF, Adachi M, Lai CK, Soriano JB, Vermiere, PA, Weiss, KB, Weiss ST (2004). Worldwide severity and control of asthma in children and adults: the global asthma insights and reality surveys. Journal of Allergy and Clinical Immunology. 114(1): 40 – 47. https://doi.org/10.1016/j.jaci.2004.04.042
Partridge MR, van der Molen T, Myrseth SE, Busse WW (2006). Attitudes and actions of asthma patients on regular maintenance therapy:
the INSPIRE study. BMC Pulmonary Medicine. 6: 13.
Hassan T, Alam MM, Wahab A, Hawlader MD (2020). Prevalence and associated factors of internet addiction among young adults in
Bangladesh. Journal of the Egyptian Public Health Association 2020; 95 : 3. https://doi.org/10.1186/s42506-019-0032-7
van der Meer V, Bakker MJ, van den Hout WB, Rabe KF, Sterk PJ, Kievit J, Assendelft WJJ, Sont JK, SMASHING Study Group (2009). Internet-based self-management plus education compared with usual care in asthma: a randomized trial. Annals of Internal Medicine. 151(2): 110–120.
https://doi.org/10.7326/0003-4819-151-2-200907210-00008
Price D, Fletcher M, van der Molen T (2014). Asthma control and management in 8,000 European patients: the REcognise Asthma and Link to Symptoms and Experience (REALISE) survey. NPJ Primary Care Respiratory Medicine 2014; 24: 14009. https://doi.org/10.1038/npjpcrm.2014.9
Schultz JM, Cooper JL, Baingana F, Oquendo MA, Espinel Z, Althouse BM, Marcelin LH, Towers S, Espinola M, McCoy CB, Mazurik L, Wainberg ML, Neria Y, Rechkemmer A (2016). The role of fear-related behaviors in the 2013-2016 West Africa Ebola Virus Disease outbreak. Curr ent Psychi a try Reports. 18: 104. https://oi.org/10.1007/s11920-016-0741-y
Ahmad S, Ismail NE (2015). A qualitative study exploring the impact of stigma in the lives of adult asthma patients in Selangor Malaysia. International Journal of Pharmacy and Pharmaceutical Sciences. 7(7): 373-375.
Beyan AC, Demiral Y, Erdal S (2018). Occupational diseases as a metaphor: do not cough! European Respiratory Journal. 52 (Suppl. 62): PA1215. https://doi.org/10.1183/13993003.congress-2018.PA1215
D'Amato G, Vitale C, Molino A, Stanziola A, Sanduzzi A, Vatrella A, Mormile M, Lanza M, Calabrese G, Antonicelli L, D'Amato M (2016). Asthma-related deaths. Multidisciplinary Respiratory Medicine. 11: 37 .https://doi.org/10.1186/s40248-016-0073-0
Weatherall M, Wijesinghe M, Perrin K, Harwood M, Beasley R (2010). Meta-analysis of the risk of mortality with salmeterol and the effect of concomitant inhaled corticosteroid therapy. Thorax. 65(1): 39 - 43. https://doi.org/10.1136/thx.2009.116608
Becker JM, Rogers J, Rossini G, Mirchandani H, D'Alonzo GE Jr (2004). Asthma deaths during sports: report of a 7-year experience. Journal of Allergy and Clinical Immunology. 113(2): 264-267. https://doi.org/10.1016/j.jaci.2003.10.052
Vermeulen F, Garcia G, Ninane V, Laveneziana P(2016). Activity limitation and exertional dyspnea in adult asthmatic patients: what do we now? Respiratory Medicine. 117: 122 - 230. https://doi.org/10.1016/j.rmed.2016.06.003
Lee S, Kirking DM, Erickson SK (2003). Methods of measuring asthma severity and influence on patient assignment. Annals of Allergy, Asthma & Immunology. 91(5): 449 - 454. https://doi.org/10.1016/S1081-1206(10)61512-8
Kendrick AH, Higgs CM, Whitfield MJ, Laszlo G (1993). Accuracy of perception of severity of asthma: patients treated in general practice. British Medical Journal. 307: 422. https://doi.org/10.1136/bmj.307.6901.422
Cowen MK, Wakefield DB, Cloutier MM (2009). Classifying asthma severity: objective versus subjective measures. Journal of Asthma. 44(9): 711 - 715. https://doi.org/10.1080/02770900701595576
Scherzer R, Grayson MH (2018). Heterogeneity and the origins of asthma. Annals of Allergy, Asthma & Immunology. 121(4): 400-405.
Published
How to Cite
Issue
Section
License

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.





